Millions of Americans suffer from fatigue, weight gain, depression, and cognitive impairment. Many believe that they have no choice but to accept these seemingly “age-related” declines in quality of life. Underactive thyroid (hypothyroidism) is often overlooked or misdiagnosed and can be the underlying cause of these symptoms.
~ Lifeextension.com
Hypothyroidism is definitely a major stress. Subnormal body temperature and too little thyroid hormone can reduce the strength and resistance of every cell, including the billions involved in the immune system.
~ Stephen Langer, MD, Solved: The Riddle of Illness
Do you feel like you’re completely falling apart? If so, now may be a good time to learn about the function of your all-important thyroid gland, how to determine whether it is slowing down, and natural ways to support it so you can start feeling healthier. This two-part article will provide you the basics of this expansive topic to start your journey to greater wholeness.
The Important Function of the Thyroid Gland
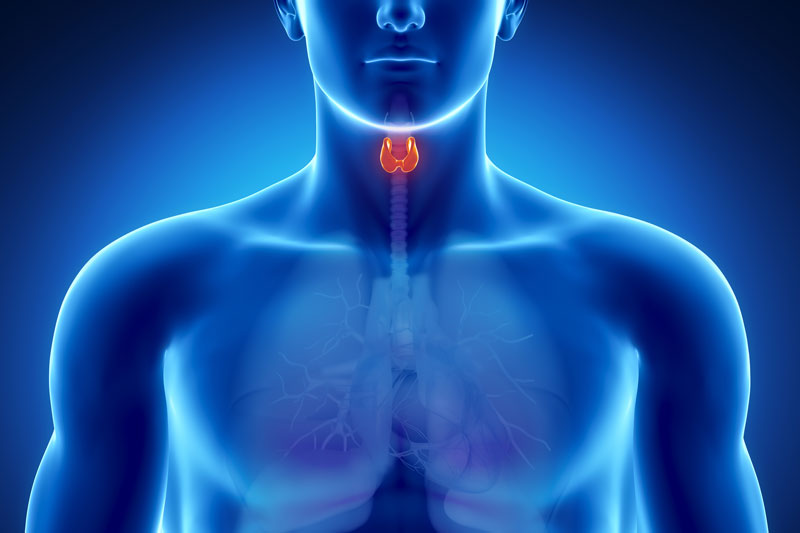
The tiny thyroid gland is butterfly-shaped and semi-circles the windpipe just below the Adam’s apple. It is made up of small sacs filled with thyroglobulin, an iodine-rich protein, and the thyroid hormones thyroxine (T4) and triiodothyronine (T3, in smaller amounts). Outside the thyroid, three selenium-dependent enzymes (iodothyronine de-iodinases) convert T4 to T3, the biologically active form of thyroid hormone (TH), but nutrient deficiencies, prescription drugs, and chemical toxicity can interfere with this conversion. These hormones regulate metabolism by controlling the rate at which the body converts oxygen and calories to energy. According to Stephen Langer, MD (Solved: The Riddle of Illness), numerous well-designed studies have shown that “production of thyroid hormone can make or break a person’s health.”
The hypothalamus and pituitary glands in the brain regulate the production of T4 and T3 (each molecule has four and three iodine atoms respectively). When the blood level of TH falls below normal, the hypothalamus releases thyroid-releasing hormone (TRH), which in turn causes the pituitary to release thyroid-stimulating hormone (TSH), which causes the thyroid to start working. When TH levels are adequate, TSH production decreases, which then slows the thyroid gland’s release of new TH.
Multiple naturally occurring biological factors can hinder TH activity: (1) T4 also converts to reverse T3 (rT3), an inactive form of T3 that blocks the thyroid hormone receptors in the cell, thus blocking activity of regular T3; (2) most THs (99%) circulating in the blood are metabolically inactive because they are bound to carrier proteins, and only the minute amount of “free” TH (mostly T3) is biologically active and binds to and activates TH receptors (even the slight changes in the amount of thyroid carrier proteins that can be produced by oral contraceptives, pregnancy, and conventional hormone replacement therapy, can lower available free TH); and (3) since even mild adrenal gland dysfunction can interfere with the steady, efficient conversion of T4 to T3, “the adrenal glands must be strengthened for thyroid supplementation to be effective” [Langer; symptoms of adrenal dysfunction include allergies/ asthma/breathing issues, skin issues (acne, eczema, psoriasis, flakiness/dryness), arthritic pains, and emotional swings].
Diagnosing Hypothyroidism: Symptoms & Tests
Hypothyroidism exists in both women and men when the thyroid gland fails to make enough THs, which results in lowered metabolic rate (slowed heartbeat, lowered blood pressure, sluggish circulation). The key symptoms of hypothyroidism are: subnormal temperature/increased sensitivity to cold; fatigue/weakness; muscle cramps; digestive problems/chronic constipation; weight gain; dry skin; brittle nails; hair brittleness/lifelessness/loss; infections and slowed wound healing; slow thinking/poor memory; persistent depression and anxiety; female problems (menstrual irregularities, infertility); and diminished/nonexistent appetite and sexual desire.
Unfortunately, since these symptoms can take years to surface, a condition called early/mild, or subclinical, hypothyroidism (SCH – without definite or readily observable symptoms) can commonly go undiagnosed with tests that show elevated TSH (0.5 – 9 µIU/mL) but normal T4 and T3 levels. Since those with early hypothyroidism are at greater risk for developing overt hypothyroidism, Kenneth Ain, MD, director of the Thyroid Oncology Program at the University of Kentucky, maintains that doctors should screen certain patients for SCH, including: (1) those with family histories of thyroid disease; (2) women who are planning pregnancy, pregnant, or have just given birth; (3) women over age 40, with PMS or perimenopause symptoms, or diagnosed with premature menopause; (4) anyone over age 60; (5) those with depression, chronic fatigue syndrome, fibromyalgia, a non-thyroid autoimmune disease, or declining kidney function. Hashimoto’s thyroiditis (autoimmune inflammation of the thyroid) is the most common cause of SCH.
Hypothyroidism and SCH are also associated with: high cholesterol, triglycerides, and blood pressure; atherosclerosis; increased risk of cardiovascular disease; increased inflammation; weakness of the immune and respiratory systems (due to reduced white blood cell activity); iron-deficiency anemia (due to decreased production of circulating blood cells in response to lowered tissue oxygen needs); and metabolic syndrome.
Traditional thyroid function tests and their interpretations are controversial, do not always tell the whole story, and can thus be misleading. It is therefore important to examine the thyroid with more than a single test, and blood test criteria for thyroid disease should serve as only one parameter. Doctors have multiple tests available for thyroid disease diagnosis, including:
1. Thyroid-Stimulating Hormone (TSH): While TSH level has long been the favored thyroid dysfunction test, the strategy for its use in diagnosis has been debated and changed over the past 10 years. No single TSH measurement should be deemed conclusive, and TSH alone should not be used to determine medication dosing.
Part of the difficulty in relying on TSH values lies in the fact that they fluctuate with various factors, including time of day (higher in the morning than in the afternoon), infection (increases TSH synthesis), seasons (rises during colder months, drops in the warmest months), a rise in estrogen (from pregnancy, birth control pills, or hormone replacement therapy), head injuries (which can damage the hypothalamus and pituitary glands), and fasting (decreases TSH).
The “normal” diagnostic TSH references available to clinicians generally range from 0.45-4.50 µIU/mL, and different medical/scientific associations and academies differ on acceptable upper limits. Studies suggest an optimal range of 0.5-2.0 µIU/mL since TSH above 2.0 may be associated with increased cardiovascular risk, and values below the normal range suggest TH excess (hyperthyroidism or Grave’s disease).
2. Free T4 & T3 (Normal FT4 = 0.7-1.9 ng/dl) (Normal FT3 = 230-619 pg/d) In symptomatic hypothyroidism, both will be below normal.
3. Reverse T3: A patient may test normal for T4 and T3, but still display hypothyroid symptoms, due to excess production of rT3. Stress and extreme exercise can both elevate rT3 levels and suppress TSH and T3 production.
4. Basal Body Temperature (Normal = 97.8 -98.2º F): A thermometer is tucked into the underarm for ten minutes immediately after waking in the morning and before rising from bed. Practitioners who use this test maintain that 2-5 consecutive days of readings below 97.8 º indicates hypothyroidism. According to Langer, this test is clinically more accurate than blood tests in patients whose symptoms suggest hypothyroidism, but whose blood work says otherwise.
5. TRH (used with caution in asthma and ischaemic heart disease patients; should not be used in pregnant women) Although TSH testing has largely replaced this test in conventional medicine, there is recent evidence that this may be a valuable diagnostic tool in many SCH patients showing high-normal TSH and low-normal or low Free T4.
6. Autoimmune Antibodies [AgAb antibodies (antithyroglobulin) and TPOAb (thyroperoxidase antibodies)] – It is most prudent, along with standard thyroid testing, to test for Hashimoto’s thyroiditis. It is important to test specifically for the blood proteins that the body produces against the thyroid gland when this condition exists. Those who are celiac or gluten sensitive are especially prone to developing Hashimoto’s, and those with chronic hives often have elevated thyroid antibodies.
The Hypothyroid Diet
Follow the following dietary guidelines to support healthy thyroid function. Eliminate beef (unless organic, grass fed), pork, lamb, and pro-inflammatory refined sugars, dairy, grains, and gluten (in wheat, barley, and rye; a TH imposter that the immune system attacks with antibodies). Consume: (1) only modest quantities of otherwise very healthy organic soy, walnuts, and organic cruciferous vegetables (cabbage, cauliflower, kale, broccoli, Brussels sprouts; these foods reduce the amount of iodine available for synthesizing T4 and T3); (2) only healthy, anti-inflammatory fats (coconut and olive oils, high omega-3 fatty acids in wild-caught fish, avocados, sprouted chia/flax/hemp seeds; almonds/walnuts/Brazil nuts soaked overnight); (3) iodine-rich organic seaweed (kelp, dulse, nori) (Note: iodine intake exceeding 800 mcg/day can lead to SCH); (4) high amounts of mineral- and fiber-rich vegetables and low-sugar berries; and (5) chicken, turkey, and eggs.
Thyroid awareness, thorough thyroid testing, and diet modification are critical first steps to reversing hypothyroidism. Watch for Part 2 of this article, which will address the dietary supplements and other lifestyle choices that can set you on the path to true, long-term thyroid wellness.
The statements in this article have not been evaluated by the Food and Drug Administration and are not intended to take the place of a physician’s advice.
Submitted by J. Erika Dworkin, Certified Lifestyle Educator and Nutrition Consultant and co-owner of the Manchester Parkade Health Shoppe (860.646.8178, 378 Middle Turnpike West, Manchester, CT, www.cthealthshop.com,) trusted since 1956. Erika is available to speak to groups.
All statements in this article are research-based and references are available upon request.